The National Aids Council (NAC) has made a deliberate effort to incorporate cancer into the response to HIV. This follows the realisation that 60% of all new cancer cases are HIV-related. NAC has been programming for cancer prevention and management. In Zimbabwe, cancer is a major cause of morbidity and mortality, with over 5 000 new diagnosed cases and over 1 500 deaths per year.
There are cancers which are more likely to occur in people who are infected with the human immunodeficiency virus (HIV) and these are classified as Aids-related cancers. The most common Aids-related cancers are Kaposi Sarcoma, Non-Hodgkins Lymphoma, Primary Central Nervous System (CNS) Lymphoma and Cervical Cancer.
These cancers, however, can also affect people who are HIV-negative. Other less-common types of Aids-related cancers include cancers of the mouth, throat, liver, lung, colon, rectum, anus, testes, and skin. The most common cancers in Zimbabwe are Kaposi’s Sarcoma, prostate cancer, oesophageal and liver cancers among men, and cervical cancer, Kaposi’s Sarcoma, breast and oesophageal cancers among women, indicating an important burden of infectious related cancers among both sexes.
Cancer occurs when cells in a specific part of the body begin to reproduce uncontrollably and the number of cancer cases has been increasing in the past few years, particularly for cancers related to infectious agents such as bacteria or virus. Statistics indicate that the vast majority of Zimbabweans diagnosed with cancer will die of the disease if no treatment is availed to them early enough.
We will be giving out information on various types of cancer in the coming weeks. For this week, we bring you information on cervical cancer.
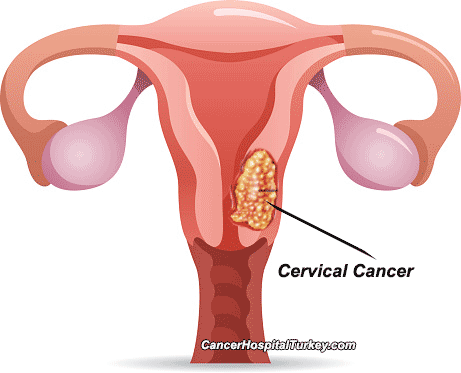
The trouble with cervical cancer
Cervical cancer is the leading cause of cancer-related illness and death in women in Zimbabwe. Women with HIV infection are more likely to also have a concurrent human papillomavirus (HPV) infection, which causes cervical cancer.
Some studies suggest that HIV infection causes rapid progression of cervical cancer from the first stage to later stages.
- Chamisa under fire over US$120K donation
- Mavhunga puts DeMbare into Chibuku quarterfinals
- Pension funds bet on Cabora Bassa oilfields
- Councils defy govt fire tender directive
Keep Reading
Easily prevented
Cervical cancer affects more than 11 000 women worldwide annually. Cervical cancer is one of the most preventable types of cancer and women can be screened for it with routine Pap tests or Visual Inspection with Acetic Acid and Camera (Viac). Cervical cancer is almost always caused by genital HPV infection.
Cervical cancer may be prevented through the HPV vaccine or treated if detected early by a regular Pap test. If abnormal cells caused by HPV are found while they are still pre-cancerous, they can be treated before they progress into cancer.
This is why it’s important for all women to have a regular Pap test, and for women 30 and older to routinely be tested for HPV as well.
No signs or symptoms
The trouble with early cervical cancer is that it generally shows no signs or symptoms. This is why regular screening is so important. A woman may develop symptoms only when the cancer has become invasive and spreads to nearby tissue.
When this happens, the most common symptoms are: abnormal vaginal bleeding; unusual discharge from the vagina (separate from your normal menstrual period); bleeding following intercourse, douching, or after a pelvic exam; and pain during intercourse. And often by this time, it is already too late to treat.
Diagnosed too late
As much as 95% of cervical cancer patients in African countries are diagnosed at late- or end-stage disease. The delayed diagnosis for these patients is due to the low level of cancer awareness between the population and the health workers, culture and constraints on access to specialised care, usually non-existent in these countries.
Most of the efforts and help provided by the Western countries to Africa are used to prevent and cure infectious diseases and malnutrition, leaving the patients with cancer to their poor destiny.
In fact, oncology in Africa seems to be a branch of the medicine that is practised only by the local traditional healers, procuring devastating effects on the natural history of the tumours.
Black women most likely to die
Based on surveys conducted by the black Women’s Health Imperative, it was found that a majority of black women are familiar with certain facts about cervical cancer — how it is caused and that it is preventable. Yet black women are still dying at a disproportionately higher rate.
Although cervical cancer occurs most often in hispanic women, black women tend to have lower five-year survival rates and die more often than any other race. In fact, black women have twice the cervical cancer mortality rate compared to white women.
New research explains why black women are more likely than whites to develop and die from cervical cancer: They seem to have more trouble clearing HPV, the virus that causes the disease. Racial differences have been noted with HPV-caused cervical cancer, with African-American women not only being more likely to develop this type of cancer, but also almost two times more likely to die from it, compared to European American women, according to the Associated Press.
Estimated rates of death from the cancers in east and southern Africa are from 30 to 60 deaths per 100 000 women, higher than in the rest of sub-Saharan Africa (20 to 35 deaths per 100 000 women).
What you should do
“For the case of cervical and ovarian cancers, women need to be keen on their periods and discharge. In case of any abnormality or persistent abdominal pains, they should go for a medical check-up immediately,” says John Ncube, a local gynaecologist.
If it is detected early, cervical cancer is one of the most successfully treatable cancers, which is why it is important to know and understand the risk factors for developing cervical cancer. However, most women wait till the cancer is at its worst stage, when only palliative care can be given, hence the increased deaths from cervical cancer.
Get screened for HIV and cancer before it is too late!! Visit your nearest health centre and find out where you can get screened. If diagnosed with any of the two conditions, or both, take treatment as prescribed by health experts.











