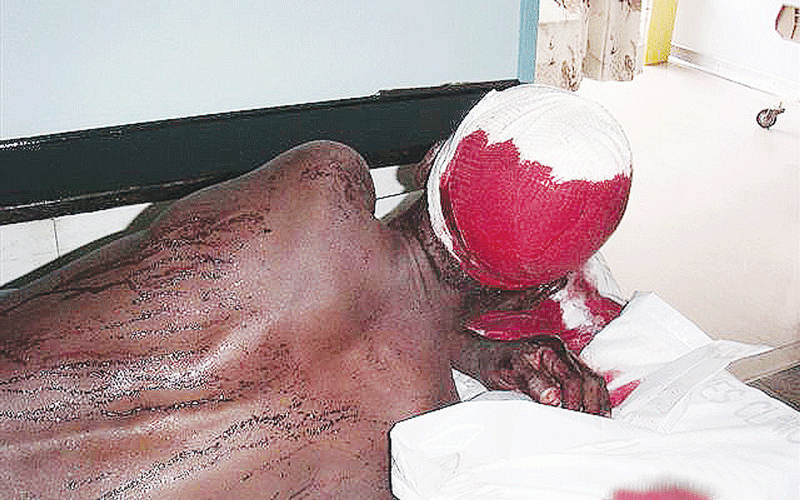
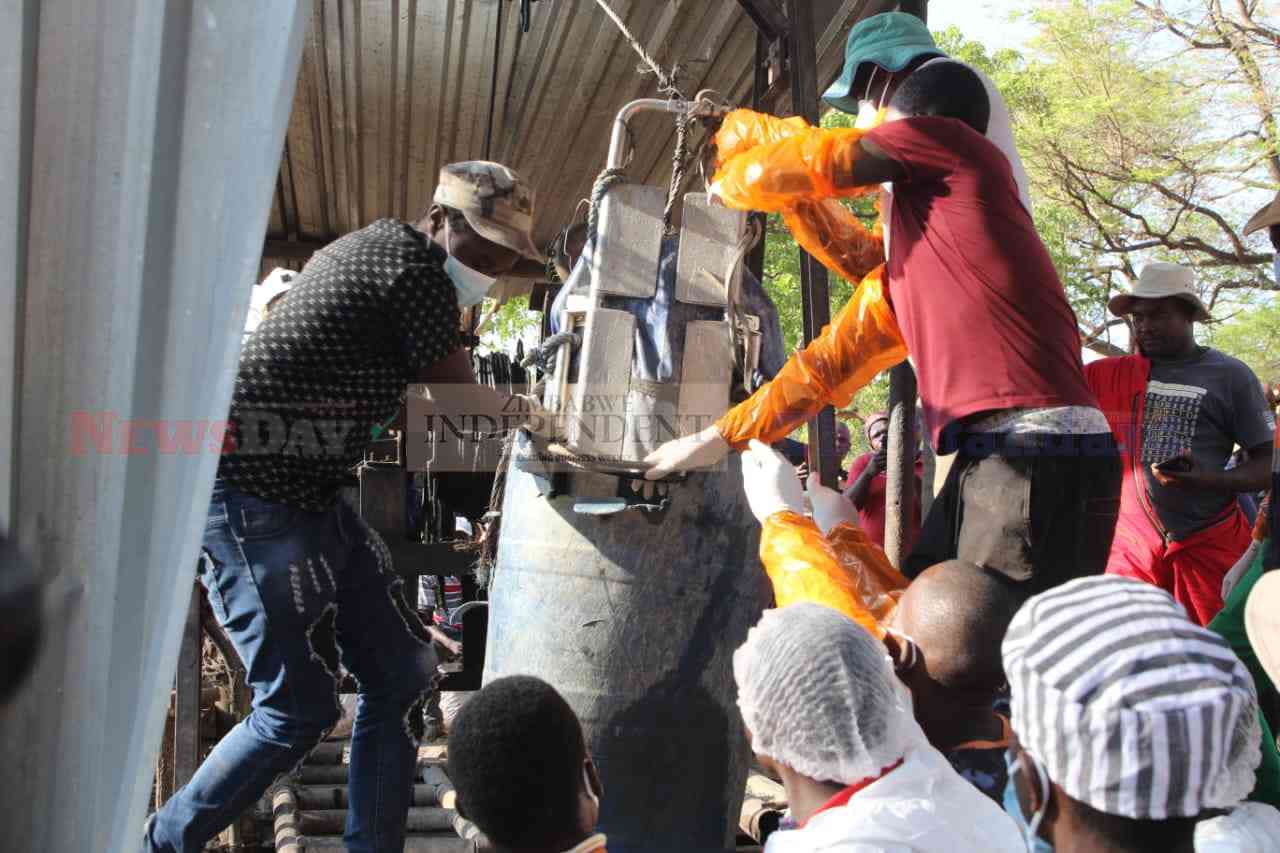Chiwenga gives voters chilling warning

Banks brace for drought-induced shocks
Winky D incident was yet another own goal
Videos
Pamela Marwisa In Conversation With Trevor
‘Embrace index insurance to combat climate change’
Coping with drought through WFP’s resilience programme
DeMbare delight at fan boost
[ad_1] Ndiraya says the support of the fans will have a huge impact on how the teams will perform this weekend. The post DeMbare delight at fan boost appeared first on NewsDay Zimbabwe. [ad_2] Source link
2021/22 PSL fixtures out – NewsDay Zimbabwe
[ad_1] BY FORTUNE MBELE THE 2021/22 Castle Lager Premier Soccer League (PSL) season fixtures were released yesterday with matches set to kick off on Saturday. Giants Dynamos will host Yadah on Match Day 1 while champions FC Platinum will also be home to new boys Tenax as Highlanders hit the road for a date with […]
Highlanders record under threat

Beyond boundaries





InnBucks, beyond what meets the eye
Ceteris Paribus: Is ZSE poised to preserve value?
Govt gifts Byo with textile manufacturing firm
Gwanda water crisis deepens
Celebrate, preserve culture for future generations: Ndinde